Applications
Hydrogels: The Future of Wound Care
Sinan Gölhan
Founder & CEO at GelTech Labs
Every year, millions of people suffer from chronic wounds.
Diabetic ulcers. Burns. Pressure injuries. Surgical wounds.
These injuries are not just painful. They are incredibly difficult to heal and can lead to infection, amputation, and significant healthcare costs.
For decades, wound care largely relied on simple dressings: gauze, bandages, and antiseptics.
Today, that paradigm is changing.
And the most promising technologies leading that change is hydrogels.
Why wounds struggle to heal
Healing skin is more complex than simply covering an injury.
Successful healing requires a delicate environment:
Moisture balance
Protection from infection
Controlled inflammation
Oxygen and nutrient transport
Cell migration and tissue regeneration
Traditional dressings often fail to maintain these conditions. They can dry out the wound, adhere to tissue, or fail to prevent bacterial growth.
Hydrogels offer a very different approach.
What makes hydrogels special
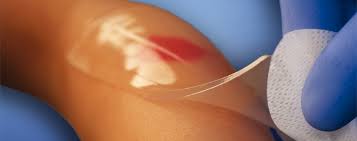
Hydrogels are polymer networks that can hold large amounts of water while maintaining a soft, solid structure.
This unique structure allows them to mimic the physical properties of natural tissue.
Their high water content helps maintain a moist wound environment, which is critical for faster healing and reduced scarring. (1)
Unlike traditional dressings, hydrogels can also be engineered to:
Deliver drugs or antimicrobial agents
Absorb wound exudate
Reduce pain during dressing changes
Promote tissue regeneration
Researchers can even embed growth factors, cells, or antibacterial compounds directly into the material to accelerate healing. (2)
In other words, the dressing becomes more than protection.
It becomes part of the therapy.
Smart wound dressings are emerging
The field is moving even further.
New hydrogel systems are being designed to actively interact with wounds.
Some advanced hydrogels can:
Kill bacteria and break down biofilms
Reduce inflammation and oxidative stress
Promote new blood vessel formation
Respond to the wound environment
For example, researchers recently demonstrated hydrogel dressings with antibacterial and antioxidative functions that accelerate healing in infected diabetic wounds. (3)
These types of materials are transforming wound care from passive treatment into active bioengineering.
Why this matters
Chronic wounds are a massive global health problem.
Diabetic foot ulcers alone affect millions of patients and are one of the leading causes of non-traumatic amputations.
Studies show hydrogel dressings can improve healing outcomes compared to conventional dressings in many cases. (4)
As materials science advances, hydrogels are becoming more sophisticated, combining multiple functions in a single platform.
Antibacterial protection.
Drug delivery.
Tissue scaffolding.
Moisture regulation.
All in one material.
The bigger shift
Historically, wound care focused on covering injuries.
The future will focus on engineering the healing environment.
Hydrogels are a perfect example of this shift. They blur the line between biomaterial and therapy.
They are soft, adaptable, and biologically compatible.
Most importantly, they help recreate the conditions the body needs to repair itself.
And that may be the biggest breakthrough of all.

